Search
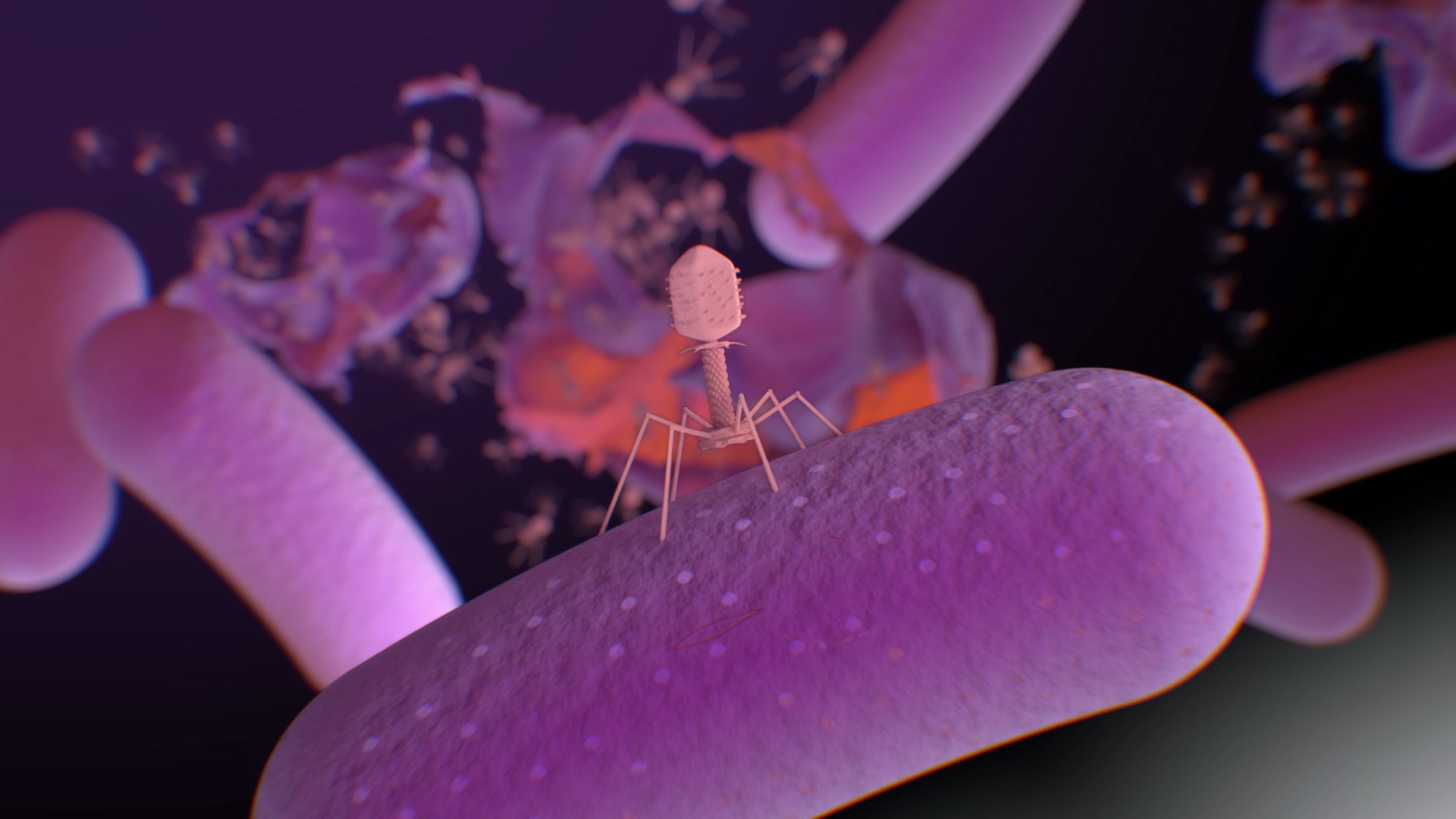
Meet the team at Phage WA, who are working to tackle antimicrobial resistance (AMR) through phage therapy.

Our team uses AI to quickly analyse large amounts of genetic data to help discover alternate medications and improve existing treatments.

As part of our research development and planning we invite members of the community to work with us. Click here to find out how.

If you have any questions or would like more information about the Western Australian Epithelial Research Program (WAERP), please click here to access our contact details.

Scientists at The Kids Research Institute Australia are taking their fight against antibiotic- resistant superbugs to the Goldfields working alongside local Indigenous communities and councils.

For decades, cystic fibrosis (CF) meant a life shaped by daily treatments, frequent hospitalisations, and an uncertain future. The arrival of CFTR modulators has changed that picture dramatically, and researchers at the Wal-yan Respiratory Research Centre now want to understand the bigger picture.
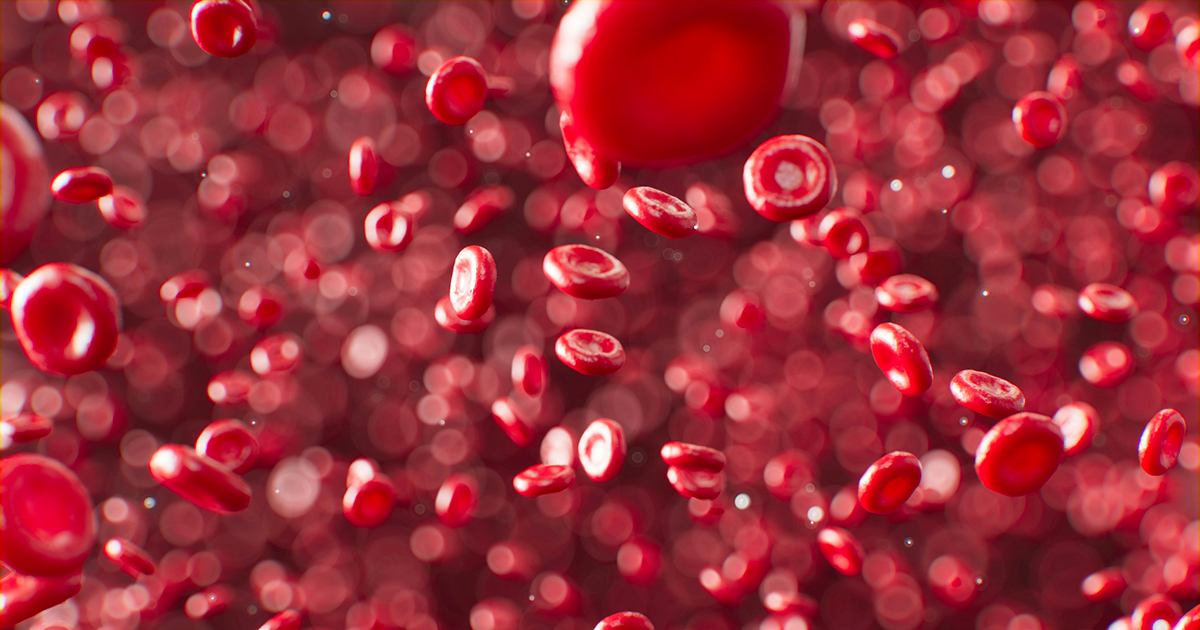
Rising carbon dioxide levels are being detected within the human body, with new research warning a key blood marker for the gas could near its healthy limit within decades if current trends continue.

Researchers developing a world-first treatment that targets an underlying cause of asthma have secured a $499,640 grant from the Future Health, Research and Innovation Fund – Innovation Seed Fund.

Dr Renee Ng, a microbiologist specialising in bacteriophage therapy – an alternative to antibiotics to fight antimicrobial resistance – will travel to the world’s premier conference on viruses, bringing new ideas, connections and expertise back to Perth.
New hope is on the horizon for people living with cystic fibrosis.
