Search
In light of the obesity epidemic, we aimed to characterize novel childhood adiposity trajectories from birth to age 14 years and to determine their relation...
Rates of type 2 diabetes are higher among Indigenous than non-Indigenous Australian children and adolescents.
To analyze the incidence of type 1 diabetes in 0- to 14-year olds in Western Australia, from 1985 to 2002, by region and socioeconomic status.
If the gut becomes damaged it may not be able to process the foods that we eat as well as it used to. This may also affect how we look after diabetes.
This study is looking for the causes of type 1 diabetes, so that we can find ways to prevent it. We will follow many women around Australia during pregnancy until early childhood, looking at the child's birth, environment and genes.
A register which stores demographic and clinical data on all patients attending the diabetes clinic at Princess Margaret Hospital
To conduct an analysis of children with TIDM’s cognitive profile at an age in which both cognition and cortical development are still maturing
Investigating changes in retinopathy, aortic intima media thickness & heart rate variability, indicators of macrovascular disease & autonomic neuropathy
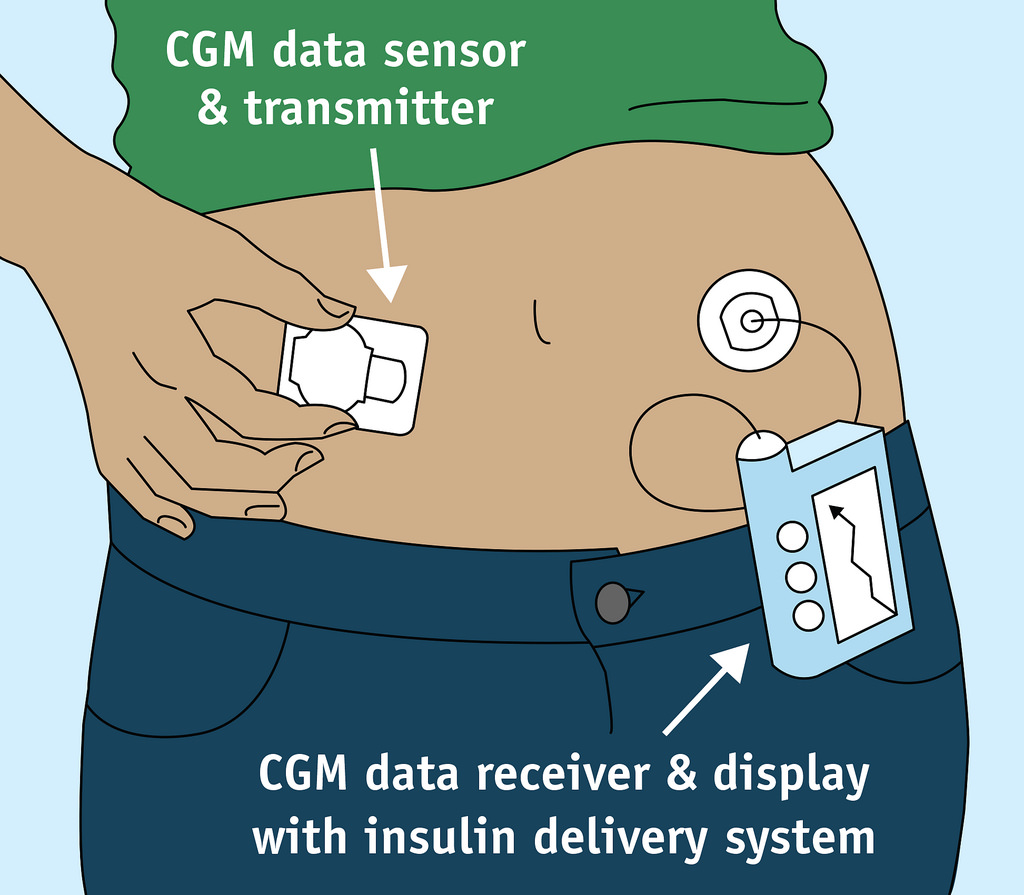
A Closed-Loop System will potentially have a major impact upon acute and chronic complications of diabetes as well as upon their quality of life.
This study will evaluate the effect of two types of aerobic exercise
