Search

Valued at a total of $440,000, the Wal-yan Respiratory Research Centre Inspiration Awards 2022 will support five cutting-edge research projects.

Two outstanding researchers from the Wal-yan Respiratory Research Centre have been awarded a 2022 Innovation Fellowship supported by the WA Government's Future Health Research and Innovation (FHRI) Fund.
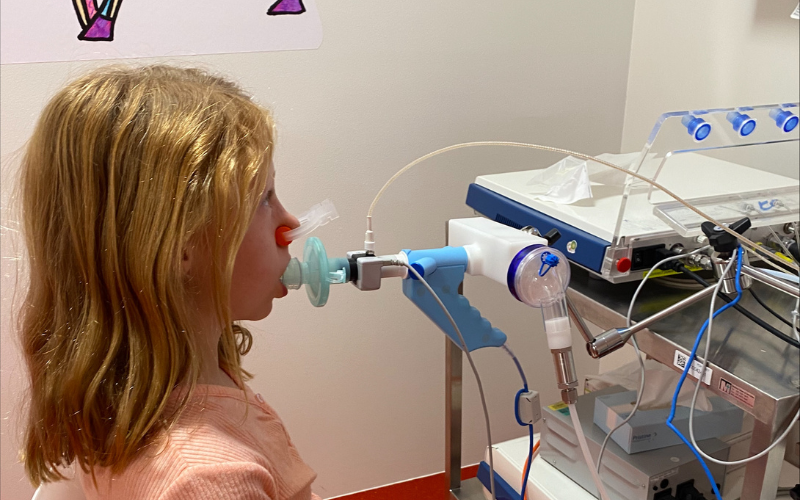
A new research project – the WA Paediatric Bronchiectasis Cohort Study – officially commenced this month with the aim of looking at children with bronchiectasis in Western Australia, like nine-year-old Holly (pictured), to better understand how this disease develops during childhood.

A study which set out to determine ways to predict the long-term lung health of young adults born very preterm has shown that a childhood history of respiratory hospital admission should be a key consideration in the management of preterm children and adults.

Dr Daniel Laucirica, a research officer with the Wal-yan Respiratory Research Centre, will undertake new research into potential treatment strategies to prevent lung damage in people with cystic fibrosis (CF), under the mentorship of Associate Professor Anthony Kicic - made possible by a Vertex Cyst

WA researchers will use a $1.97 million Medical Research Future Fund grant to develop a strategy for better follow-up of First Nations children after they’ve been hospitalised for respiratory infections, in a bid to halt the slide into more severe lung disease.
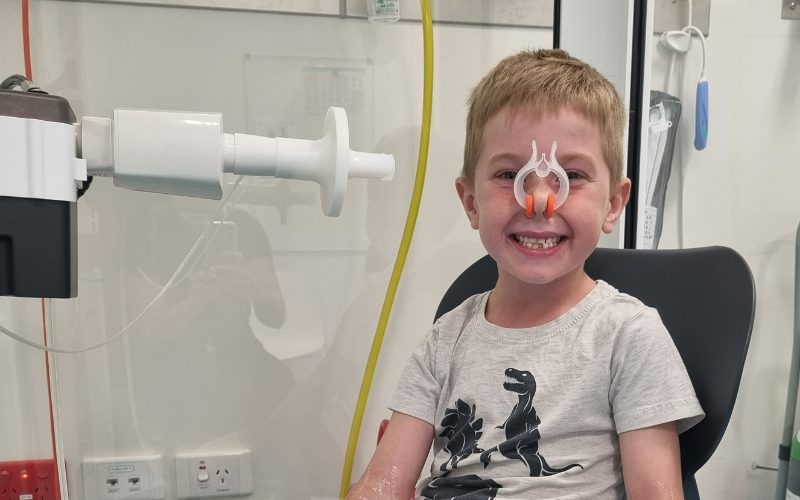
A new study to determine if it’s safe for children who were born preterm to attend day care officially commenced this month.

A co-designed and culturally secure intervention to improve medical follow-up for Aboriginal children hospitalised with acute chest infections resulted in higher follow-up rates and improved longer-term lung health outcomes for children.

Flare-ups of asthma are usually brought on by respiratory infections, such as the common cold, and are one of the most common reasons for a child to miss school or require emergency care.

A new study has found a common asthma drug is effective for some very premature babies who go on to suffer from lung complications.
